Burning Feet at Night: Causes, Fixes, and When to See a Clinician
You finally get into bed, the house goes quiet, and then it starts: burning feet that feel hot, prickly, raw, or oddly electric against the sheets. Patients often ask me whether this automatically means diabetic nerve damage. Not always. But it is a symptom that deserves a closer look, especially when it keeps showing up at night, starts affecting sleep, or comes with numbness, balance problems, skin changes, or a sore that is not healing. In my clinic, the real question is not just why the feet burn. It is what pattern the symptom fits, and how fast someone needs to act.
Burning Feet at Night: What This Symptom Usually Means
Burning feet at night are a symptom, not a diagnosis. That matters because the same sensation can come from several different pathways. In one person, it may be irritated peripheral nerves. In another, it may be inflamed skin, fungal infection, pressure from shoes, or a circulation issue. The body does not label the signal for you. It just sends distress.
Here is the pattern I see most often in diabetes care: the burning starts in the toes or soles, shows up more in the evening, and may be paired with tingling, numb patches, stabbing zaps, or a weird sensitivity to bedsheets. That combination pushes peripheral neuropathy higher on the list when someone reports burning feet most nights. Night can amplify the feeling because there are fewer distractions, less movement, and more light contact from bedding. What feels manageable during the day can feel a lot louder once everything gets still.
At the same time, not every case belongs in the neuropathy box. If there is itching, peeling, cracking between the toes, or a rash-like flare after sweaty shoes, skin disease moves up the list. If one foot suddenly looks redder, hotter, or more swollen than the other, that changes the urgency. The first job is to notice the pattern, because recurring burning feet often tell a different story than a one-off flare after a long day.
What Diabetic Neuropathy Can Feel Like Early On
When people hear neuropathy, they often imagine severe pain or complete numbness right away. Real life is usually messier than that. Early diabetic nerve damage can feel subtle. Some people notice a faint burning in the soles. Others feel pins-and-needles, buzzing, random zaps, or the sense that their socks are bunched up even when they are not.
In my clinic, patients often describe three early patterns. First, the feet feel hot at night even when they are cool to the touch. Second, the sheets hurt, which can happen when light touch starts triggering pain. Third, they notice less feeling in some areas, even while other areas burn. That mix of pain plus reduced sensation is one reason clinicians take the complaint seriously. Pain gets attention, but numbness raises the risk of missing a blister, cut, or pressure injury.
Another clue is symmetry. Diabetic peripheral neuropathy often starts in both feet in a stocking-like pattern. It may creep upward slowly. It can also affect balance, especially in the dark, because the brain gets poorer feedback from the feet. Readers who want a deeper breakdown of diabetic neuropathy symptoms, stages, and healing can use that wider framework to understand how early nerve changes differ from advanced loss of sensation.
Causes of Burning Feet Beyond Diabetes Alone
Diabetes is a major cause, but it should not become a lazy catch-all explanation. The symptom deserves a differential diagnosis. One of the most practical examples is vitamin B12 deficiency. That matters because long-term metformin use can lower B12 levels in some people, and low B12 can add to neuropathy symptoms.
Skin conditions matter too. Athlete’s foot can burn, sting, itch, peel, and crack. Contact irritation from soaps, creams, or sweaty footwear can also make the soles feel inflamed. Mechanical stress is another overlooked issue. Shoes that are too narrow, too stiff, or rubbing the same pressure point every day can turn a small problem into a nightly one. The National Institute of Diabetes and Digestive and Kidney Diseases also notes that doctors often check for thyroid problems, kidney disease, or low vitamin B12 levels when nerve symptoms do not fit a simple one-cause story.
Circulation fear is common, and sometimes justified. But the pain pattern is different more often than people realize. Poor circulation classically causes exertional cramping, nonhealing wounds, color changes, or a cold foot, rather than simple nighttime burning alone. Alcohol-related nerve injury, thyroid disease, kidney disease, and some medications can also be part of the story. That is why good medicine does not stop at one assumption.
Sleep-Friendly Fixes and At-Home Relief for Burning Feet
People want practical relief, and that is fair. Nighttime foot burning can wreck sleep, patience, and quality of life. The first rule is simple: do not use aggressive heat on feet that may have reduced sensation. Heating pads, very hot water, and direct heat can backfire because the skin may not register injury normally.
A cooler sleep setup often helps when burning feet are being amplified by heat and friction. Breathable socks, lighter bedding over the feet, and avoiding overheated rooms can make the symptom less intense. If sweating and friction are part of the picture, moisture-wicking socks and shoes with a roomier toe box can reduce irritation. Some people also feel better after a brief cool-not-ice rinse, followed by careful drying, especially between the toes.
This is also a good time for a nightly foot check. Look for cracks, blisters, redness, peeling, pressure marks, swelling, or a nail problem. If vision or flexibility makes that tough, use a mirror or ask for help. That habit sounds basic, but it catches a surprising number of problems early.
What a Clinician Will Usually Check for Burning Feet
A good evaluation for this symptom is not usually dramatic. It is detailed. The clinician will want to know when the symptoms started, whether both feet are involved, whether there is numbness, whether the skin has changed, what medicines you take, and whether there are clues pointing beyond diabetes alone. That history helps separate classic burning feet from skin-only irritation or a more urgent vascular problem.
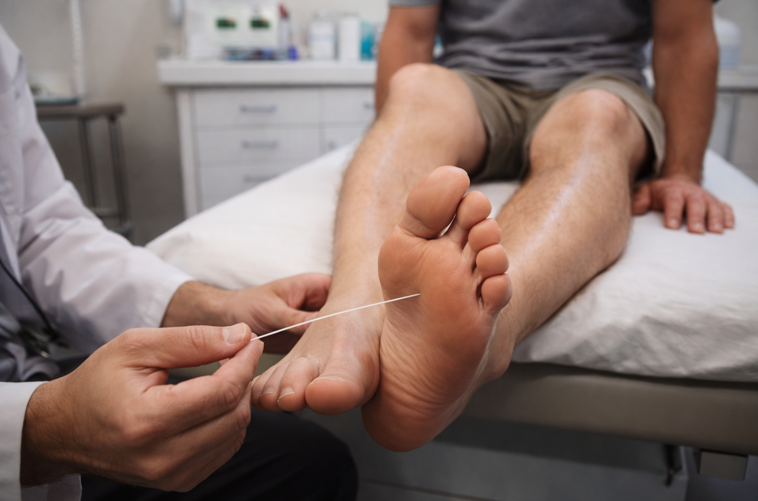
The foot exam itself matters a lot. A clinician may look at skin integrity, pulses, temperature differences, deformities, calluses, fungal changes, and pressure points. They may test sensation with a monofilament, vibration, or pinprick. If the story sounds atypical, they may order labs to look at vitamin B12, thyroid function, kidney function, or other contributing factors.
Patients often assume they need a nerve study right away. Usually they do not. In many straightforward cases, the pattern, history, and physical exam tell most of the story. Extra testing becomes more important when symptoms are one-sided, suddenly worsening, strongly affecting strength, or not fitting the usual neuropathy pattern. The CDC foot-care guidance also reinforces daily checks and regular foot exams for anyone with diabetes-related foot symptoms.
When Burning Feet Need Faster Attention
Some versions of this symptom can wait for a routine clinic visit. Others should not. If the foot is suddenly red, hot, swollen, or changing shape, that is not something to brush off. Infection and Charcot-related change are two reasons clinicians move quickly in a diabetic foot.
A sore, blister, or cut that is draining, smells bad, or is surrounded by spreading redness also deserves prompt care. So does a foot that turns pale, blue, unusually cold, or sharply painful. Those signs point away from a simple symptom-management conversation and toward a more urgent limb-safety conversation.
Even without obvious skin damage, it is worth booking a visit if burning feet are getting more frequent, waking you up, or coming with dizziness on standing, bowel or bladder changes, or sexual symptoms. Nerve problems in diabetes do not always stay confined to one body system.
See also: Treat Mental Health Nevada: Trusted Mental Health Care for Lasting Recovery
Treatment Options and What to Expect With Burning Feet
Treatment depends on cause. If the symptom is being driven by diabetic neuropathy, the plan usually has two tracks. One track is protection: foot care, glucose management, safer shoes, and addressing anything that raises ulcer risk. The second track is symptom control.
For neuropathic pain, clinicians may discuss medicines from several established categories, including gabapentinoids, SNRIs, tricyclic antidepressants, or selected topical approaches. These are not magic fixes, and one person’s that really helped can be another person’s not worth the side effects. The goal is usually to dial symptoms down, improve function, and help sleep, not promise a total reset.
If another cause is contributing, treatment needs to match that cause. That may mean addressing a fungal infection, checking for B12 deficiency, reviewing medication effects, or escalating foot protection if there is a structural problem. What usually does not help is guessing for months while the symptom keeps getting louder.
Complications People Often Miss
This symptom is uncomfortable, but discomfort is not the whole story. The bigger risk is what can ride alongside it. Numbness can make injuries easier to miss. Weak balance can raise fall risk. Chronic nighttime pain can chip away at sleep and mood. A warm swollen neuropathic foot can be mistaken for just inflammation when it actually needs urgent evaluation.
There is also a wider quality-of-life angle that people do not always mention out loud. Diabetes-related nerve and vascular changes can overlap with sleep disruption, low confidence, relationship strain, and sexual health concerns. Patients often feel awkward bringing that up, but it belongs in the conversation. A practical resource on reverse diabetic ED and recovery signs can help frame that discussion in a more informed, less panicked way, especially when neuropathy concerns are part of a bigger diabetes picture.
That does not mean every case predicts sexual dysfunction or a severe complication. It means diabetes complications often travel in clusters, and care gets better when people talk about the full pattern instead of one isolated symptom.
Protecting Your Feet Day to Day When Burning Feet Keep Coming Back
Daily prevention is not glamorous, but it works. For many people, keeping burning feet from turning into skin injury is the real win. Check your feet every day. Wash and dry them gently. Moisturize dry skin, but not between the toes if moisture is building up there. Wear socks and shoes that fit well. Do not go barefoot if sensation is reduced. Rotate footwear if sweating or pressure is a problem.
If you already have neuropathy, make foot checks part of routine life rather than an afterthought. Remove your shoes and socks during clinic visits so the feet actually get looked at. Ask about a comprehensive foot exam if you have not had one recently. That is especially important when the symptom is new, changing, or happening alongside numbness.
Patients often ask whether better glucose control will make the burning go away. Sometimes symptoms improve. Sometimes the bigger win is slowing progression, reducing complications, and making pain more manageable over time. The honest answer is that nerve symptoms do not always follow a neat script. But earlier attention usually gives you more room to respond well.
FAQ
Is nighttime foot burning always neuropathy?
No. Neuropathy is common, especially in diabetes, but skin irritation, fungal infection, pressure from shoes, vitamin deficiencies, and circulation-related problems can also cause similar symptoms.
Why do bedsheets make my feet hurt?
That can happen when irritated nerves start treating light touch as painful. It is a common neuropathic complaint, especially at night.
Can metformin play a role in nerve symptoms?
Indirectly, yes. Long-term metformin use can contribute to low vitamin B12 levels in some people, and low B12 can worsen or mimic neuropathy symptoms.
Is foot burning an emergency?
Not always. But foot burning with redness, swelling, drainage, deformity, severe color change, or a new wound should be assessed more quickly.
Should I see a podiatrist or my regular doctor first?
Either can be a good starting point. Many people begin with their primary clinician, especially if the symptom may be tied to diabetes, medications, or other whole-body issues.
Author Verification
Name: Dr. Mian Farhan Haider, MS, RD
Role: Consultant RD since 2019, with a focus on metabolic disease, diabetes, and patient-centered education.
Standard: This article is educational and editorial in nature; it does not diagnose or prescribe for individual readers.